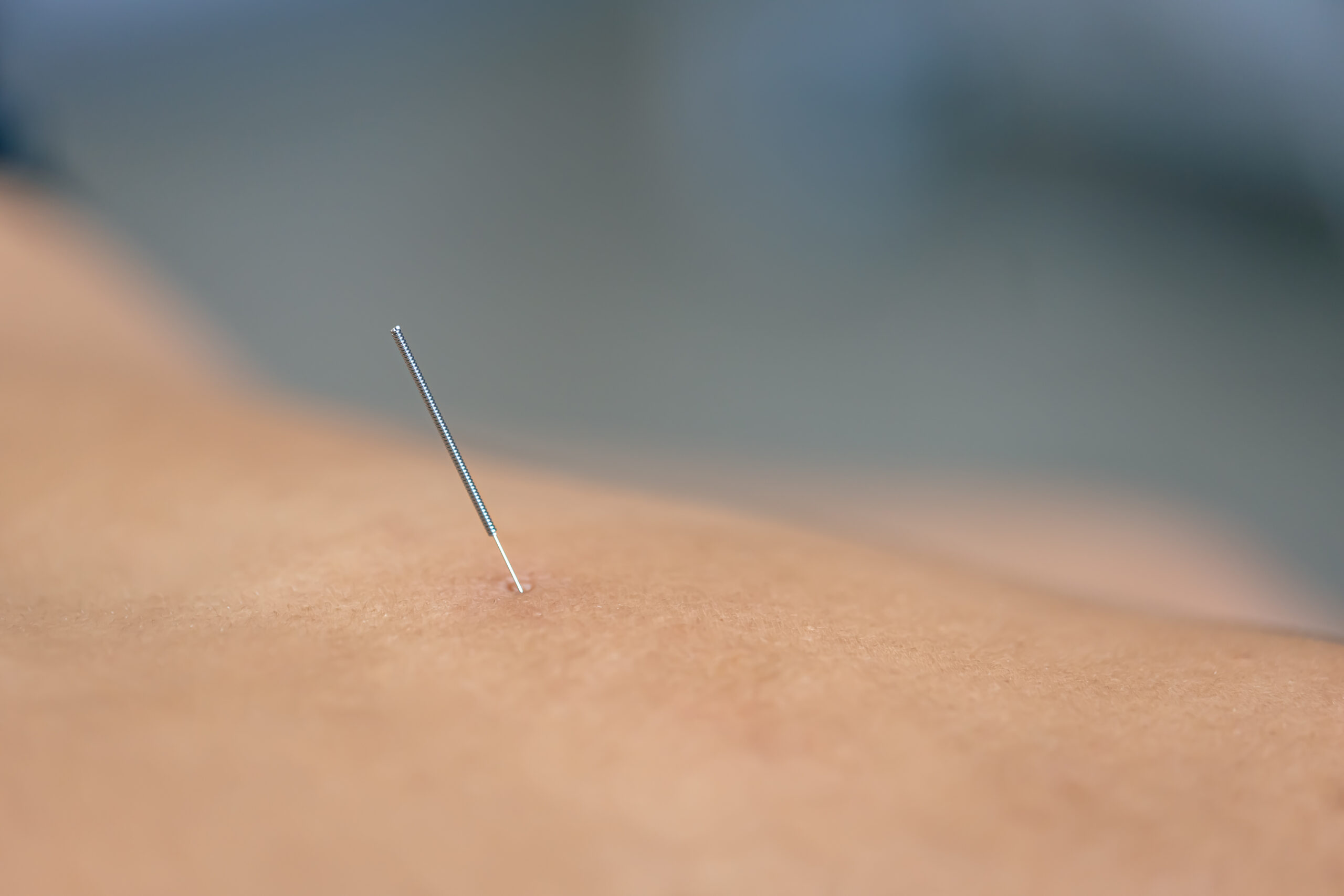
Dry needling (DN) is a technique used by physical therapists to treat musculoskeletal pain. It involves the use of thin filiform needles to stimulate trigger points in muscles and connective tissues. Several studies have investigated the efficacy of DN in pain management and muscle rehabilitation. A systematic review and meta-analysis showed that percutaneous needle electrolysis (PNE) is slightly more effective than DN in reducing pain, although the clinical significance of this difference is unclear [1] .
DN has been found to have a short-term analgesic effect in all body regions and may be of additional value when combined with other physiotherapeutic interventions [2]. Additionally, deep dry needling (DDN) has shown promise in improving range of motion and facilitating treatment for post-stroke patients with spasticity or hypertension [3]. Ultrasound-guided dry needling has also been explored for the treatment of myofascial pain, particularly in the thoracolumbar fascia [4]. Overall, DN appears to be a useful technique for pain management and muscle rehabilitation, but further research is needed to fully understand its effectiveness and optimal application.
Targeting Pain Points: How Dry Needling Relieves Muscular Tension and Discomfort
Dry needling is a minimally invasive technique that targets myofascial trigger points to relieve musculoskeletal pain [5]. It involves inserting a filiform needle into the target area, which can be classified as trigger point dry needling, fascial needling, scar tissue needling, and more [6]. The mechanism of dry needling is explained by various ideas, including increased blood flow, metabolic changes, spontaneous electrical activity, pain gating, and therapeutic current delivery to the tissues [7]. Dry needling has been shown to be effective in reducing pain intensity and improving cervical range of motion in patients with neck pain due to myofascial trigger points [8]. It elicits a neural twitch response, causing the muscle to relax and allowing for pain reduction and improvements in range of motion [9]. Dry needling is often used as a complementary medicine option to manage pain, particularly in chronic painful disease groups in the musculoskeletal system . However, more studies are needed to further explore the effectiveness of dry needling in different pain conditions .Enhancing Muscle Function: The Impact of Dry Needling on Rehabilitation
Dry needling has been shown to have a positive impact on muscle function and rehabilitation [10] [11] [12] [13]. Studies have demonstrated that dry needling, when combined with neurorehabilitation, can lead to a reduction in muscle thickness, spasticity, and reflex torque, as well as an improvement in upper extremity motor performance and dexterity in chronic stroke patients [14]. Additionally, dry needling has been found to be effective in managing postoperative shoulder pain and dysfunction following rotator cuff repair surgery . It has also been shown to improve spasticity, balance, pain, functional outcomes, and tremors in post-stroke patients . The technique involves inserting a filiform needle into the target muscle, which induces local stretch and modulates the reflex arc, leading to decreased excitability of the alpha motor neuron . Overall, dry needling is emerging as a cost-effective and beneficial technique for enhancing muscle function and improving rehabilitation outcomes in various patient populations.Comparing Dry Needling to Traditional Therapies: Effectiveness and Benefits
Dry needling (DN) has been shown to be effective in treating musculoskeletal disorders, including low back pain (LBP) [15] [16]. DN according to the Five Regulatory Systems concept (FRSc) has been found to significantly reduce pain and improve functional efficiency in LBP patients [17] [18]. It has been shown to be superior to sham/no intervention and equally effective as other interventions for short-term pain reduction in various body regions [19]. DN combined with conventional physical therapy has been found to be more effective than conventional therapy alone in reducing pain intensity, improving function, and ultrasonographic features in patients with jumper’s knee . However, there is still a need for standardization of DN protocols to address heterogeneity and strengthen the current evidence . Overall, DN shows promise as an effective treatment option for musculoskeletal disorders, but further research is needed to establish its long-term effects and optimize its use in clinical practice.Safety Considerations in Dry Needling: What Patients Should Know
Dry needling is a widely used alternative therapy for musculoskeletal disorders, such as myofascial pain. However, there are potential complications associated with the procedure, including cardiac tamponade, hematoma, infection, nerve injury, and pneumothorax [20]. It is important for patients to be aware of these potential complications as part of the informed consent process. In the case of dry needling in the upper lumbar spine, there is an increased risk of piercing the kidney, so practitioners should exercise caution and aim for a safety zone of needling less than 2.5 cm laterally from the L1 spinous process [21]. On the other hand, dry needling of the pronator teres muscle can be accurately and safely conducted using described anatomical landmarks [22]. Dry needling has shown efficacy in the management of post-stroke disability, including reducing muscle spasticity, improving functional outcomes and balance, reducing pain, and improving tremors [23]. Overall, patients should be aware of the potential complications and safety considerations associated with dry needling.Collaborative Care: Integrating Dry Needling with Other Therapeutic Modalities
Collaborative care involving the integration of dry needling with other therapeutic modalities has shown promise in various areas of healthcare. For example, in the management of lower back pain (LBP), dry needling according to the FRSc concept has been found to be effective in reducing pain and improving functional efficiency [24]. Additionally, collaborative care models have been explored for patients with musculoskeletal conditions and co-existing symptoms of anxiety and depression, with the aim of providing integrated diagnosis and treatment of mental and physical health [25]. Furthermore, dry needling has been used in post-stroke rehabilitation to address spasticity, balance, and pain, resulting in improved functional outcomes [26]. These findings suggest that integrating dry needling with other therapeutic modalities can be a valuable approach in collaborative care settings.References :
- Christos, Fakontis., Paris, Iakovidis., Dimitrios, Lytras., Konstantinos, Kasimis., Georgios, Koutras., S., R., Ntinou., Anastasios, Kottaras., Ioanna, P., Chatziprodromidou., Paraskevi, Chatzikonstantinou., Thomas, Apostolou. (2023). Efficacy of percutaneous needle electrolysis versus dry needling in musculoskeletal pain: A systematic review and meta-analysis.. Journal of Back and Musculoskeletal Rehabilitation, Available from: 10.3233/bmr-220408
- , Chys., Kayleigh, De, Meulemeester., Indra, De, Greef., Carlos, Murillo., Wouter, Kindt., Yassir, Kouzouz., Bavo, Lescroart., Barbara, Cagnie. (2023). Clinical Effectiveness of Dry Needling in Patients with Musculoskeletal Pain—An Umbrella Review. Stomatology, Available from: 10.3390/jcm12031205
- (2023). First documented effect of deep dry needling during early rehabilitation on muscle tone after thalamus hemorrhage: case report. Available from: 10.21203/rs.3.rs-2962037/v1
- Rostyslav, V, Bubnov., Lev, Kalika. (2022). Po237 / #554 the role of thoracolumbar fascia ultrasound in low back pain – guided dry needling implication. Neuromodulation, Available from: 10.1016/j.neurom.2022.08.409
- Simon, J., Padanilam., Steven, R., Dayton., Ryan, Jarema., Michael, J, Boctor., Vehniah, K., Tjong. (2021). Dry Needling for the Treatment of Musculoskeletal Ailments With Trigger Points. Available from: 10.1177/26350254211023776
- Subhanjan, Subhasis, Das., Prema, Kulkarni. (2022). Updated review on overview of dry needling. International journal of health sciences, Available from: 10.53730/ijhs.v6ns1.5991
- , G.., Anil, K., Gupta., Dileep, Kumar., Sudhir, R, Mishra., Ganesh, Yadav., Madhumita, Singha, Roy., Laxmi, Prajapti. (2023). Efficacy of Dry Needling Versus Transcutaneous Electrical Nerve Stimulation in Patients With Neck Pain Due to Myofascial Trigger Points: A Randomized Controlled Trial. Cureus, Available from: 10.7759/cureus.36473
- , G.., Anil, K., Gupta., Dileep, Kumar., Sudhir, R, Mishra., Ganesh, Yadav., Madhumita, Singha, Roy., Laxmi, Prajapti. (2023). Efficacy of Dry Needling Versus Transcutaneous Electrical Nerve Stimulation in Patients With Neck Pain Due to Myofascial Trigger Points: A Randomized Controlled Trial. Cureus, Available from: 10.7759/cureus.36473
- Karle, Kotze. (2019). The Pairing of Trigger Point Dry Needling with Rehabilitation Techniques.
- Fatemeh, Panahi., Samaneh, Ebrahimi., Zahra, Rojhani-Shirazi., Ladan, Hemmati. (2023). Effects of neurorehabilitation with and without dry needling technique on muscle thickness, reflex torque, spasticity and functional performance in chronic ischemic stroke patients with spastic upper extremity muscles: a blinded randomized sham-controlled clinical trial.. Disability and Rehabilitation, Available from: 10.1080/09638288.2023.2190168
- (2023). First documented effect of deep dry needling during early rehabilitation on muscle tone after thalamus hemorrhage: case report. Available from: 10.21203/rs.3.rs-2962037/v1
- Mehdi, Dadgoo., Mohammad, Reza, Pourahmadi., Morteza, Nakhaei, Amroodi., Pouria, Tabrizian., Ali, Ahmadzadeh, Amiri. (2023). Dry needling in a multimodal rehabilitation protocol following rotator cuff repair surgery: study protocol for a double-blinded randomized sham-controlled trial. BMC Musculoskeletal Disorders, Available from: 10.1186/s12891-023-06269-1
- (2022). The Emergence of Dry Needling in Stroke Rehabilitation. Available from: 10.56536/sjptr.v2i.13
- Nirmal, Surya., Guhan, Ramamurthy. (2022). Dry needling in stroke. Exploration of Neuroprotective Therapy, Available from: 10.37349/ent.2022.00016
- Joanna, Rajfur., Katarzyna, Rajfur. (2023). Dry needling according to the FRSc concept performed on the cruciate and pelvic ligaments in lower back pain: a case report. Medical Science Pulse, Available from: 10.5604/01.3001.0053.6731
- , Chys., Kayleigh, De, Meulemeester., Indra, De, Greef., Carlos, Murillo., Wouter, Kindt., Yassir, Kouzouz., Bavo, Lescroart., Barbara, Cagnie. (2023). Clinical Effectiveness of Dry Needling in Patients with Musculoskeletal Pain—An Umbrella Review. Stomatology, Available from: 10.3390/jcm12031205
- Faiza, Sharif., Ashfaq, Ahmad., Syed, Amir, Gilani. (2023). Effectiveness of ultrasound guided dry needling in management of jumper’s knee: a randomized controlled trial. Dental science reports, Available from: 10.1038/s41598-023-31993-y
- Guan-Yuan, Jin., Louis, Lei, Jin., Bonnie, Xia, Jin. (2023). The necessity of inheritance and innovation of classical acupuncture from the rising of dry needling. World journal of acupuncture-moxibustion, Available from: 10.1016/j.wjam.2023.05.005
- Joanna, Rajfur., Katarzyna, Rajfur., Łukasz, Kosowski., Karolina, Walewicz., Robert, Dymarek., Kuba, Ptaszkowski., Jakub, Taradaj. (2022). The effectiveness of dry needling in patients with chronic low back pain: a prospective, randomized, single-blinded study. Dental science reports, Available from: 10.1038/s41598-022-19980-1
- César, Fernández-de-las-Peñas., Carlos, López-de-Celis., Jacobo, Rodríguez-Sanz., César, Hidalgo-García., Joseph, M, Donelly., Simón, A, Cedeño-Bermúdez., Albert, Pérez-Bellmunt. (2021). Safety of Dry Needling of the Pronator Teres Muscle in Cadavers: A Potential Treatment for Pronator Syndrome.. Pain Medicine, Available from: 10.1093/PM/PNAB274
- Niyati, Patel., Manali, Patel., Brian, Poustinchian. (2019). Dry Needling–Induced Pneumothorax. The Journal of the American Osteopathic Association, Available from: 10.7556/JAOA.2019.009
- Nirmal, Surya., Guhan, Ramamurthy. (2022). Dry needling in stroke. Exploration of Neuroprotective Therapy, Available from: 10.37349/ent.2022.00016
- Cody, J, Mansfield., Cody, J, Mansfield., M, Harr., Matthew, S., Briggs., James, A., Onate., James, A., Onate., Laura, C., Boucher., Laura, C., Boucher. (2020). Safety of dry needling to the upper lumbar spine: a pilot cadaver study.. Journal of Manual & Manipulative Therapy, Available from: 10.1080/10669817.2019.1708593
- Richard, Colbran. (2022). Collaborative Care – working with community to plan primary health services.. International Journal of Integrated Care, Available from: 10.5334/ijic.icic22020
- Joanna, Rajfur., Katarzyna, Rajfur. (2023). Dry needling according to the FRSc concept performed on the cruciate and pelvic ligaments in lower back pain: a case report. Medical Science Pulse, Available from: 10.5604/01.3001.0053.6731